TL;DR:
- Case conceptualization provides a personalized story connecting your history, strengths, and current challenges.
- It guides therapy by identifying patterns, triggers, and cultural factors for tailored interventions.
- Active client involvement in co-creating the conceptualization enhances therapy effectiveness and collaboration.
Many therapeutic breakthroughs start not with a formal diagnosis, but with mapping the unique web of experiences, relationships, and beliefs that shape who you are. Most people assume therapy is primarily about naming what’s wrong. In reality, the most meaningful progress often comes from building a rich, personalized picture of your life, your patterns, and your strengths. That process is called case conceptualization, and it changes everything about how treatment feels and works. In this guide, we’ll break down what case conceptualization is, how therapists use it, how different therapy models approach it, and why your active involvement makes all the difference.
Table of Contents
- What is case conceptualization?
- How therapists use case conceptualization
- Comparing conceptualization frameworks
- Case conceptualization for complex or diverse cases
- A fresh perspective on case conceptualization
- Connect with supportive Bergen County therapists
- Frequently asked questions
Guide Overview: Key Sections on Case Conceptualization
| Point | Details |
|---|---|
| Holistic insight | Case conceptualization provides a big-picture view that helps tailor therapy to your personal needs. |
| Collaborative approach | Working with your therapist on your conceptualization leads to better outcomes and deeper understanding. |
| Framework comparisons | Different therapy models have unique ways of conceptualizing challenges, each offering valuable perspectives. |
| Cultural sensitivity | A good conceptualization respects your cultural, social, and personal context for authentic support. |
What is case conceptualization?
Case conceptualization is essentially your therapist’s working map of you. It goes far beyond a checklist of symptoms. Instead, it weaves together your personal history, current challenges, cultural context, relationships, and inner strengths into a coherent story that explains why you feel the way you do and how to help you move forward.
Think of it this way: two people can share the same diagnosis yet need completely different approaches to healing. One person’s anxiety might trace back to early childhood instability. Another’s might stem from a high-pressure career and unresolved grief. A diagnosis tells you what is happening. A case conceptualization tells you why, and points toward how to address it effectively.
Case conceptualization is foundational for effective therapy, integrating clients’ history, context, and vulnerabilities into a usable clinical framework. That integration is what makes your treatment plan feel tailored rather than generic.
A thorough case conceptualization typically includes several key elements:
- Personal and family history: Early experiences, attachment patterns, major life events
- Current symptoms and concerns: What you’re struggling with right now, and how it shows up day to day
- Behavioral and emotional patterns: Recurring cycles that may be keeping you stuck
- Strengths and protective factors: The resilience, relationships, and resources already working in your favor
- Cultural and social context: How your identity, community, and environment shape your experience
- Triggers and vulnerabilities: Specific situations or stressors that intensify your challenges
This map isn’t fixed. It evolves as your therapist learns more about you and as you gain insight yourself.
Pro Tip: Don’t hesitate to ask your therapist directly, “What’s your current conceptualization of my situation?” Most therapists welcome that question. It deepens the collaboration and helps you feel like a partner in your own healing rather than a passive recipient of care.
How therapists use case conceptualization
Knowing what a case conceptualization is matters less than understanding how it actually shapes your therapy experience. This is where the framework goes from an abstract idea to something you can feel in every session.
Here’s a simplified look at how therapists typically apply it:
- Gathering your story: The first few sessions are largely about listening. Your therapist collects information about your history, relationships, current symptoms, and goals.
- Identifying patterns: Therapists look for recurring themes, such as avoidance, self-criticism, or difficulty setting boundaries, that connect your past experiences to present challenges.
- Building a working hypothesis: Based on what they learn, your therapist develops an initial conceptualization. This is their best current explanation of what’s driving your struggles.
- Sharing and refining together: Good therapists don’t keep this map to themselves. They share it with you, invite your feedback, and adjust it based on what resonates or doesn’t.
- Guiding interventions: Every technique your therapist uses, whether it’s a breathing exercise, a thought record, or a conversation about your past, is chosen because it targets something identified in your conceptualization.
The most skilled therapists make this process empirically grounded, collaborative, and culturally sensitive, steering clear of a deficit-only lens that reduces you to your problems.
“Case conceptualization is most powerful when it is collaborative and avoids pathologizing.”
Cultural sensitivity deserves a special mention here. A therapist skilled in conceptualization recognizes that your background, values, and community aren’t just context. They’re central to understanding you. For example, someone exploring trauma therapy approaches will find that culturally aware conceptualization dramatically improves how relevant and effective those approaches feel.
Comparing conceptualization frameworks
Not all therapists approach case conceptualization the same way. The therapy model a clinician uses shapes how they interpret your story, what they pay attention to, and how they design your treatment. Understanding the differences helps you find the approach that fits you best.
The three most common frameworks are Cognitive Behavioral Therapy (CBT), humanistic and existential therapy, and the Power Threat Meaning (PTM) Framework. Each has a distinct lens:
| Framework | Core focus | How it shapes conceptualization | Client experience |
|---|---|---|---|
| CBT | Thoughts, behaviors, and their connections | Maps cognitive distortions and behavioral patterns | Structured, goal-oriented, skill-building |
| Humanistic/Existential | Personal meaning, identity, and growth | Centers your narrative and life purpose | Reflective, open-ended, deeply personal |
| PTM Framework | Social power, context, and meaning-making | Focuses on “what happened to you” not “what’s wrong with you” | Validating, socially aware, empowering |
CBT focuses on mechanisms and functional analysis, humanistic therapy prioritizes narrative, and the PTM Framework centers on social context and meaning.
Here’s a quick guide to when each framework tends to shine:
- CBT works particularly well when you have specific, identifiable patterns of anxious thinking or avoidance. You can explore a solid CBT overview to see if it aligns with your needs.
- Humanistic/Existential therapy suits people navigating identity questions, major life transitions, or a loss of meaning and purpose.
- PTM Framework is especially valuable if you’ve experienced systemic disadvantage, discrimination, or social trauma. A thorough CBT guide can help you compare this with cognitive approaches.
Many skilled therapists blend elements from multiple frameworks, choosing what fits your individual conceptualization rather than rigidly following one model.
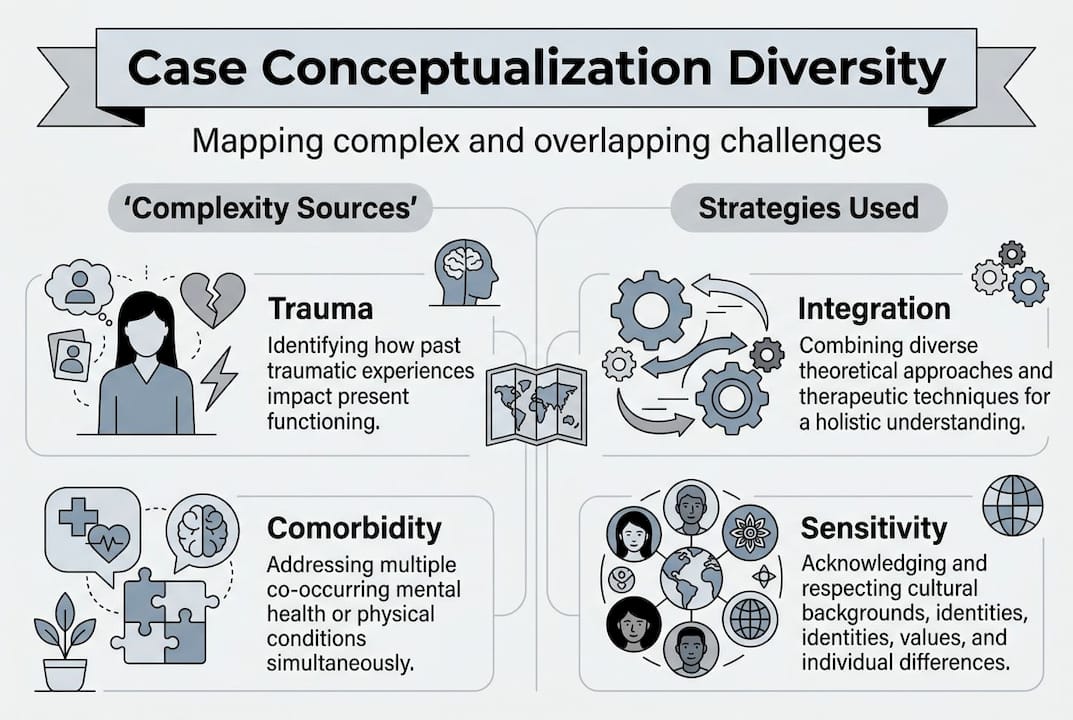
Case conceptualization for complex or diverse cases
Some situations are harder to map than others. When someone is dealing with overlapping challenges, such as trauma alongside depression and a chronic health condition, a single framework rarely tells the whole story. These are the cases where thoughtful, nuanced conceptualization matters most.
Complexity can show up in several forms:
| Source of complexity | What it means for conceptualization | Possible strategies |
|---|---|---|
| Comorbidity (multiple diagnoses) | Symptoms interact and reinforce each other | Integrated, multi-theoretical approach |
| Cultural context | Values and identity shape how distress is expressed and understood | Culturally adapted frameworks, community awareness |
| Trauma history | Past experiences filter current perceptions and responses | Trauma-informed lens across all interventions |
| Subtle vulnerabilities | Strengths mask underlying struggles | Deeper exploration beyond surface-level functioning |
Edge cases demand multi-theoretical integration, especially when cultural and complex factors intersect. This isn’t just a clinical preference. It’s what genuinely moves the needle for people who’ve felt misunderstood in past therapy experiences.
For example, someone with both trauma and significant cultural identity considerations may find that a purely CBT-based conceptualization misses crucial pieces. Exploring CBT for trauma as one component of a broader approach often yields better results than any single method alone.
Pro Tip: If your situation feels complicated, ask your provider directly: “Do you use multi-theoretical approaches?” A therapist who can adapt across frameworks is often better equipped to handle life’s real complexity, rather than fitting your story into a single model.
A fresh perspective on case conceptualization
Here’s something most therapy articles won’t tell you: the therapist’s conceptualization is only half the picture. The real breakthroughs tend to happen when you actively participate in building that map.
Many people enter therapy expecting the clinician to figure them out and deliver answers. That model puts you in a passive role and quietly reinforces the idea that you don’t fully understand yourself. The truth is that you hold enormous amounts of insight that no therapist can access without your active contribution.
Making conceptualization collaborative is vital for therapeutic success, and this is especially meaningful for Bergen County residents navigating busy, high-pressure lives. When you co-create the story of what’s driving your challenges, the resulting treatment plan feels genuinely yours, not a prescription handed down from an expert.
This shift from passive to active changes the entire arc of therapy. You stop waiting for clarity and start building it. For anyone ready to step into that kind of collaborative trauma therapy or broader personal growth work, the first step is simply asking for more involvement in your own conceptualization process.
Connect with supportive Bergen County therapists
Understanding case conceptualization is a powerful first step, and finding a therapist skilled in this approach makes all the difference in turning that understanding into real progress.
At Bergen County Therapist, Dr. Stephen Oreski and his team specialize in building personalized treatment plans rooted in thorough, collaborative conceptualization. Whether you’re exploring psychotherapy options, seeking trauma therapy, or considering the flexibility of online therapy benefits, we’re here to meet you where you are. Reach out today for a free consultation and take the next step in your personal growth journey.
Frequently asked questions
How does case conceptualization differ from diagnosis?
Case conceptualization integrates history and meaning, while diagnosis focuses on identifying and categorizing symptoms. Your conceptualization is the unique story behind those symptoms, not just a label for them.
Can a case conceptualization change over time?
Yes, absolutely. As your circumstances shift and your self-awareness grows, a good therapist updates your conceptualization to reflect a better, more accurate picture of where you are. Case conceptualization should be collaborative and adaptable throughout your time in therapy.
How is cultural sensitivity included in case conceptualization?
Therapists account for your cultural background, values, and community context to ensure the framework is relevant and respectful. Conceptualization includes cultural sensitivity and actively avoids reducing your experience to deficits or Western-centric assumptions.
Can I ask my therapist about my case conceptualization?
Absolutely, and we encourage it. Asking your therapist to share their conceptualization of your situation strengthens your working relationship and deepens your self-understanding. Collaboration is key to making this process genuinely effective.
Recommended
- Individual Therapy Explained: Support and Growth with Dr Stephen Oreski & Associates.
- Individual Therapy: Transforming Personal Challenges
- Why Seek Counseling? Discover Benefits with Dr Stephen Oreski & Associates.
- 7 Key Benefits of Counseling for Personal Growth
- Why Naming Your Feelings Helps — The Caia Journal