TL;DR:
- Therapy for sexual abuse survivors follows a structured, three-phase model prioritizing safety before processing trauma.
- Evidence-based methods like TF-CBT and EMDR have strong research support for long-term effectiveness.
- Pace, individual readiness, and self-care are key; healing is non-linear and tailored to each survivor.
Deciding to seek therapy after sexual abuse is one of the most courageous steps a survivor can take, and it’s also one of the hardest. The uncertainty of what therapy will look and feel like can stir up fear, shame, and doubt before you’ve even made the first call. If you’re a Bergen County resident trying to understand what the process actually involves, this guide is for you. We’ll walk through how to prepare, what the phased therapy model looks like, which evidence-based methods are available, and how to handle the rough patches along the way.
Table of Contents
- What to know before starting sexual abuse therapy
- Step-by-step: The three phases of sexual abuse therapy
- Evidence-based therapy methods: What are your options?
- Troubleshooting challenges and adapting therapy
- Supplemental supports: Self-care, groups, and community healing
- A therapist’s perspective: Why slow and steady wins the healing race
- Next steps: Finding therapy and support in Bergen County
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Therapy follows three phases | You’ll move through safety, remembrance, and reconnection steps at your own pace during therapy. |
| Multiple therapy options exist | Evidence supports methods like TF-CBT and EMDR, but the right approach is unique to each person. |
| Non-linear progress is normal | Ups and downs are expected—steady support and community help your healing journey. |
| Adapting therapy is okay | Therapists provide different methods and pacing to meet your needs if progress stalls or feels unsafe. |
| Local and national support available | If you’re in Bergen County, resources and groups can help you start your recovery process. |
What to know before starting sexual abuse therapy
With the emotional weight of beginning therapy in mind, let’s start with key preparations and what you should expect before your first session.
Many survivors worry they’ll be asked to relive every traumatic detail from day one. That’s a myth worth dismantling right now. The standard therapy process for adult survivors follows a structured, phased model that begins with safety, not disclosure. No competent trauma therapist will push you to go deeper than you’re ready to go.
You don’t need to feel “ready” in any perfect sense. You just need enough willingness to try. Common signs that someone is ready to begin include:
- Experiencing distress that is affecting daily functioning, sleep, or relationships
- Having some basic life stability, such as safe housing or a support system
- Feeling even a small desire to feel better
- Being able to commit to attending sessions regularly
Before your first appointment, it also helps to think through a few practical considerations:
- What are your goals? Reducing anxiety? Processing specific memories? Improving relationships?
- What’s your schedule? Weekly sessions are most common, so consider availability.
- What are your boundaries? You have the right to set the pace in therapy.
- Do you have a crisis plan? Know who to call or where to go if sessions bring up intense feelings between appointments.
Part of finding a good fit means learning how to go about finding a sexual abuse therapist who specializes in trauma. Not every licensed counselor has trauma-specific training, and that distinction matters enormously.
Pro Tip: You are allowed to interview multiple therapists before committing. Ask about their experience with trauma survivors, their therapeutic approach, and how they handle disclosures. If something feels off in the consultation, trust that instinct.
It’s also worth knowing that many survivors carry shame or worry about disclosing past abuse to a partner as part of their broader healing process. Therapy can support that, too, when the time is right.
Step-by-step: The three phases of sexual abuse therapy
Once you’ve prepared mentally and practically, understanding the structure of effective therapy can help demystify the process.
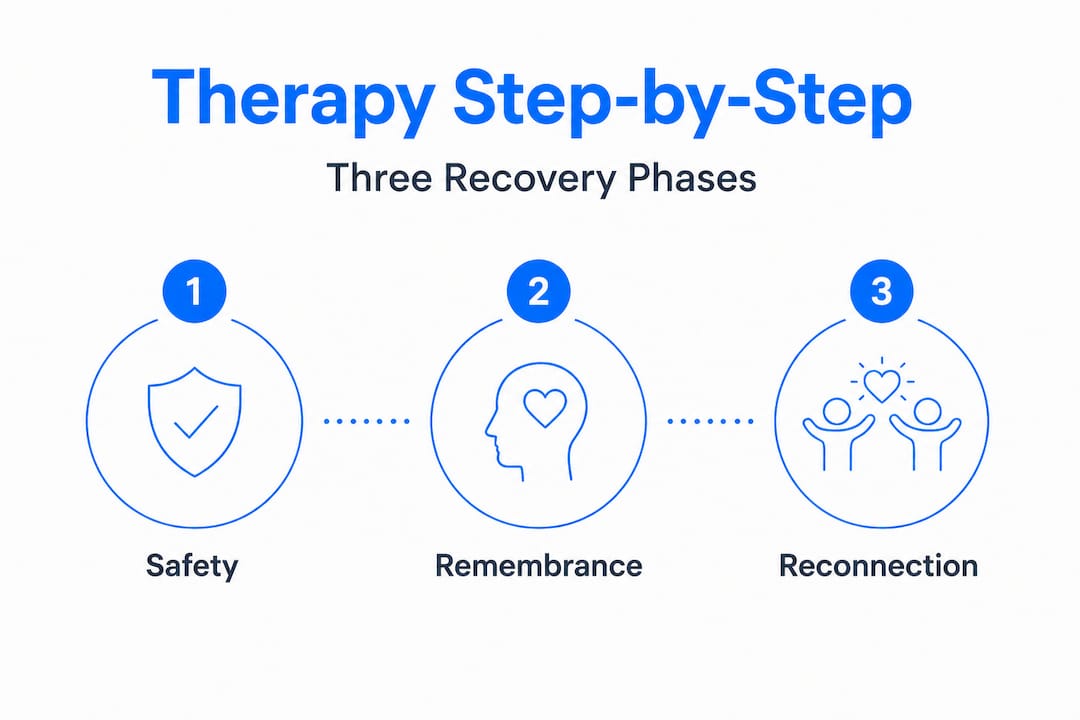
The standard therapy model for adult survivors uses a three-phase approach developed over decades of clinical research. Understanding each phase takes away some of the fear of the unknown.
-
Safety and stabilization — This is always the starting point. The goal is to build coping skills, establish trust with your therapist, and create emotional regulation tools before touching traumatic memories directly. This phase might involve breathing exercises, grounding techniques, and safety planning.
-
Remembrance and mourning — Once you have stable coping tools, therapy may move toward gently processing traumatic memories. This doesn’t mean replaying every detail. It means making meaning of what happened, expressing grief, and beginning to release the emotional charge of the past.
-
Reconnection and integration — The final phase focuses on rebuilding your sense of self, relationships, and future. Survivors often describe this stage as reclaiming their identity beyond the trauma.
| Phase | Main goal | Typical tasks | Signs of progress |
|---|---|---|---|
| Safety and stabilization | Build a foundation | Coping skills, grounding, trust | Reduced crisis episodes, feeling safer |
| Remembrance and mourning | Process the trauma | Narrative work, grief, meaning-making | Less emotional reactivity to memories |
| Reconnection and integration | Rebuild your life | Identity work, relationships, future goals | Engaging with life again, renewed purpose |
One critical insight: high dropout risks exist in trauma-focused therapy, particularly for complex cases. Phased approaches are specifically designed to reduce those risks by not rushing survivors into painful material before they have the tools to handle it.
Pro Tip: Progress is not a straight line. It is completely normal, and expected, to revisit earlier phases. If life stress spikes or a new trigger surfaces, stepping back to stabilization is a sign of good self-awareness, not failure. You can learn more about phased therapy approaches and how they apply to your situation.
Evidence-based therapy methods: What are your options?
Knowing the structure of therapy, the next question is which therapeutic approaches are available and evidence-based for sexual abuse recovery.
Evidence-based methodologies include Trauma-Focused CBT (TF-CBT), EMDR, Prolonged Exposure (PE), Cognitive Processing Therapy (CPT), and mindfulness and body-focused therapies. Each has a different focus and works better for certain survivors.
| Therapy method | Primary focus | Best for | Typical duration |
|---|---|---|---|
| TF-CBT | Thoughts, feelings, behaviors | Children, adolescents, adults | 12-25 sessions |
| EMDR | Processing traumatic memory | Adults with vivid trauma memories | 6-12+ sessions |
| Prolonged Exposure (PE) | Reducing avoidance | PTSD with avoidance patterns | 8-15 sessions |
| CPT | Challenging unhelpful beliefs | Guilt, shame, self-blame | 12 sessions |
| Somatic and mindfulness | Body and nervous system | Body-stored trauma, dissociation | Ongoing |
Notably, TF-CBT and EMDR show sustained effects beyond one month after treatment ends, while other approaches have more limited long-term data. That doesn’t make others invalid; it simply means those two have the most robust research backing. A broader review of PTSD and depression intervention effectiveness consistently supports these modalities for sexual trauma specifically.
Before committing to a method, consider asking your therapist:
- Have you used this approach with sexual abuse survivors specifically?
- What does a typical session look like with this method?
- How will we know if it’s working, and what happens if it doesn’t?
- Are there approaches you would combine with this one?
Exploring trauma therapy examples can help you understand these methods in more practical, real-world terms before you commit to any one path.
Troubleshooting challenges and adapting therapy
With an overview of popular therapy types, let’s tackle what happens when things get tough or therapy needs adapting.
Not every survivor’s path follows a tidy progression. Complex trauma, meaning repeated or prolonged abuse, often brings additional challenges such as dissociation, emotional flooding, or co-occurring conditions like depression or borderline personality disorder (BPD). These realities don’t mean healing isn’t possible. They mean the approach needs more care and flexibility.
“For edge cases like dissociation or comorbidities, use phased treatment, skills training such as DBT-PTSD, or body-focused therapies before processing traumatic memories.” Phased Treatment and Skills Training
Rushing into memory processing without stabilization can actually worsen outcomes. Research comparing trauma-focused therapy approaches for complex cases finds that phased models are preferred precisely to avoid decompensation, which is a clinical term for a sudden worsening of symptoms.
Here’s how a skilled therapist may adapt your treatment when challenges arise:
- Pause memory-focused work and return to stabilization skills when symptoms spike.
- Add DBT-based skills training to build emotional tolerance before deeper processing.
- Incorporate somatic techniques if the body is carrying the trauma more than conscious memory.
- Adjust session frequency or length to reduce overwhelm between appointments.
- Coordinate with other providers, such as a psychiatrist, if medication support is needed.
If you’re wondering how to take that first practical step, reading about starting trauma therapy can clarify what the initial process actually looks like. You can also learn more about trauma therapy in general before your first session.
Pro Tip: It is entirely okay to need pauses, to change methods, or to slow down. Speak up if something feels too intense. A good therapist will adjust without judgment.
Supplemental supports: Self-care, groups, and community healing
Often, the most sustained healing comes from a blend of techniques, support, and daily practices outside of formal therapy.
Healing is non-linear, and support groups alongside self-care practices meaningfully enhance therapy outcomes. What happens between your sessions matters just as much as the sessions themselves.
Somatic therapies such as yoga and sensorimotor psychotherapy are effective adjuncts, especially for trauma stored in the body rather than conscious memory. Survivors often describe yoga not as exercise, but as a way to reclaim a sense of safety in their own skin.
Practical supplemental supports include:
- Peer support groups, which reduce isolation and normalize the healing journey
- Mindfulness practices like meditation or breathwork to regulate the nervous system daily
- Somatic movement, including trauma-informed yoga
- Journaling, as a low-pressure way to process feelings between sessions
- Creative expression, such as art, music, or writing
- Trusted relationships with friends or family who respect your pace
For men in particular, support for male survivors offers specific resources tailored to unique barriers male survivors often face, such as stigma or disbelief. Bergen County residents can also explore group therapy options as a valuable complement to individual work. National resources at RAINN provide 24/7 hotlines and referrals if you need support outside of therapy hours.
A therapist’s perspective: Why slow and steady wins the healing race
One thing we’ve seen consistently in working with trauma survivors is the pressure people put on themselves to “get through it” quickly. Society sends messages that healing should happen fast, that therapy is about achieving breakthroughs and then moving on. That framing actually gets in the way.
There is no universal timeline for healing from sexual abuse. Some survivors stabilize within months. Others work through layers of trauma for years, and both paths are valid. What we consistently notice is that the clients who push hardest to rush into intense processing phases are also the ones who burn out or stop coming to therapy altogether. That’s not a character flaw. It’s a clinical pattern.
Therapy effectiveness depends far more on pacing and fit than on speed. A slower, well-grounded approach with a therapist you trust will outperform an aggressive, fast-tracked approach almost every time. Celebrating small milestones matters too. Being able to sleep through the night, having one less panic attack per week, or telling your story without dissociating are enormous wins. They deserve to be recognized as such.
If you’re working on finding trustworthy therapy in Bergen County, give yourself permission to take that search seriously. The right fit, found thoughtfully, changes everything.
Next steps: Finding therapy and support in Bergen County
If you’re ready to move forward, here’s how to connect to trustworthy support and get started on your healing journey in Bergen County.
At Bergen County Therapist, Dr. Stephen Oreski and our team offer trauma-specialized care for adults navigating the aftermath of sexual abuse. We provide both in-person and online sessions, meaning access to the right care doesn’t depend on your location or schedule.
Whether you’re just beginning to consider therapy or already know you want to get started, we encourage you to explore the different types of psychotherapy available and to take a look at what beginning therapy looks like with our practice. Your healing deserves a thoughtful, personalized plan, and our free consultation is the first step toward building one.
Frequently asked questions
How do I know if I’m ready for sexual abuse therapy?
You’re ready when you want change, feel safe enough to talk, and can commit to regular sessions, even if you feel nervous at first. Safety and stabilization are built into the therapy process from the very beginning, so readiness doesn’t require perfect emotional stability.
What is the best therapy type for sexual abuse recovery?
Trauma-focused CBT and EMDR are most supported by research, with sustained effects beyond one month after treatment ends. The best method ultimately depends on your specific needs, trauma history, and comfort level with different approaches.
How long does sexual abuse therapy last?
Therapy can last months or years, moving through phases based on your goals and readiness. The three-phase therapy model is not tied to a fixed number of sessions but to clinical and personal milestones.
What if therapy feels too intense or triggering?
Tell your therapist immediately. Methods and pacing can be adjusted, including pausing memory work and adding skills training first to strengthen your emotional foundation before going deeper.
Are there support groups or additional resources in Bergen County?
Group therapy options are available locally, and national resources through RAINN provide 24/7 support, hotlines, and referrals for survivors anywhere in the country.
Recommended
- How to Find a Sexual Abuse Therapist: A Guide by Dr Stephen Oreski & Associates.
- Telling Your Partner About Sexual Abuse – Dr. Stephen Oreski & Associates
- Group Therapy for Abuse: Healing Through Connection
- How to Start Trauma Therapy: A Step-by-Step Guide to Healing
- Trauma: Why the Past Keeps Showing Up in Your Present