TL;DR:
- Therapists’ emotional reactions, known as countertransference, influence therapy based on their self-awareness.
- Proper management of countertransference improves therapy outcomes and deepens the client-therapist relationship.
- Awareness, supervision, and self-reflection are key strategies for therapists to handle countertransference effectively.
Most people assume therapy is a one-way street where only the client’s emotions are under the microscope. But therapists are human, too, and they bring their own histories, biases, and emotional responses into every session. These reactions, known as countertransference, can quietly shape the direction of therapy in ways that are either deeply helpful or subtly harmful. Understanding what countertransference is, how it shows up, and how skilled therapists manage it gives both clients and professionals a clearer picture of what makes therapy truly effective.
Countertransference Guide: Sections at a Glance
- Defining countertransference: From Freud to modern therapy
- How countertransference shows up: Types and examples
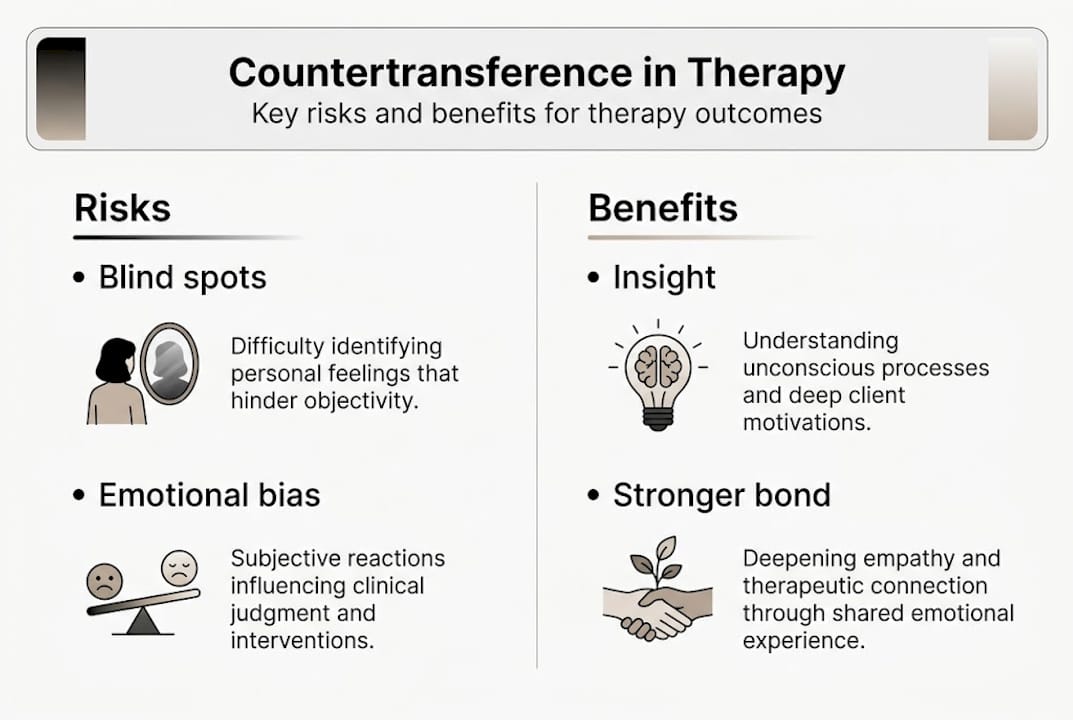
- Why countertransference matters: Risks, benefits, and real impacts
- Managing countertransference: Best practices for clients and professionals
- Special challenges: Countertransference in trauma and complex cases
- A fresh look: Why embracing countertransference leads to better therapy
- Find supportive therapy that values insight and self-awareness
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Definition matters | Countertransference describes therapists’ emotional responses to clients and is present in every therapeutic relationship. |
| Types and examples | There are many forms of countertransference, each influencing how therapy unfolds in unique ways. |
| Manage, don’t avoid | The goal is not to eliminate countertransference but to recognize and manage it for better therapy outcomes. |
| Special cases stand out | Countertransference intensifies in trauma and complex cases, requiring extra awareness and support. |
| Perspective shift | Embracing countertransference as a tool for insight can deepen understanding for both therapist and client. |
Defining countertransference: From Freud to modern therapy
Countertransference has been part of psychotherapy’s vocabulary for over a century, yet it remains one of the most misunderstood concepts in the field. Sigmund Freud introduced the idea in 1910, originally framing it as a problem: the analyst’s unconscious conflicts interfering with objective treatment. Back then, the prescription was simple: therapists should undergo their own analysis to clear out these reactions.
Modern therapy tells a more nuanced story. Today, countertransference is defined as the full range of a therapist’s emotional reactions, feelings, thoughts, and behaviors toward a client. It is no longer seen purely as a contaminant. Instead, it is recognized as an inevitable part of every therapeutic relationship.
“Countertransference is the therapist’s emotional reactions, feelings, thoughts, or behaviors toward the patient, originally defined by Freud in 1910.”
Every therapist, regardless of experience or training, will experience countertransference. What separates effective clinicians from less effective ones is not the absence of these reactions but the awareness and management of them.
Countertransference can be:
- Positive: Feeling warmth, protectiveness, or admiration toward a client
- Negative: Experiencing irritation, boredom, dread, or even resentment
- Cognitive: Forming assumptions or judgments about a client’s choices
- Behavioral: Subtly changing body language, tone, or session structure in response to a client
For clients, this means that a well-trained therapist is not a blank screen. They are an active participant in the relational dynamic, and their self-awareness directly affects how objective and supportive they can be for you.
How countertransference shows up: Types and examples
Countertransference does not wear one face. It takes on different forms depending on the therapist, the client, and the material being explored in therapy. Understanding these forms helps both professionals and clients recognize when it might be at play.
The mechanics of countertransference involve unconscious projection, where therapists can displace feelings from their own past onto a client (subjective countertransference) or react to the client’s actual behaviors (objective countertransference).
| Type | Description | Example |
|---|---|---|
| Subjective | Stems from the therapist’s own history | Feeling sad when a client discusses grief because the therapist lost a parent |
| Objective | A natural reaction to the client’s behavior | Feeling uneasy when a client is persistently hostile |
| Direct | Response to what the client does or says | Feeling flattered when a client praises the therapist excessively |
| Indirect | Response to the therapy topic itself | Feeling anxious when a client describes a traumatic event similar to the therapist’s own |
| Positive | Warmth, care, or over-identification | Wanting to protect a client like a younger sibling |
| Negative | Irritation, dread, or detachment | Feeling relieved when a difficult client cancels |
Here are some real-life scenarios therapists commonly encounter:
- A therapist who grew up with an alcoholic parent feels a surge of frustration when a client minimizes their drinking.
- A therapist feels unusually protective of a young client who reminds them of themselves at that age.
- A therapist becomes overly cheerful and avoids difficult topics with a client who seems fragile.
- A therapist dreads sessions with a client who is highly critical, reflecting the therapist’s own fear of failure.
Pro Tip: If you notice your therapist seems unusually distant, overly enthusiastic, or avoids certain topics, it may be worth gently naming what you observe. Good therapists welcome this kind of honest feedback. Exploring the benefits of seeking counseling can also help you understand what a healthy therapeutic relationship should feel like.
Why countertransference matters: Risks, benefits, and real impacts
Countertransference is not just a theoretical concept. It has direct, measurable consequences for therapy outcomes. When it goes unmanaged, it can distort a therapist’s judgment, create unhealthy dynamics, or even cause harm. When it is handled skillfully, it becomes one of the most powerful tools in the therapeutic toolkit.
Good management of countertransference strongly predicts better therapy results. This is not a minor footnote. It means that a therapist’s self-awareness is directly tied to how much progress a client makes.
Effective therapists monitor countertransference to stay objective, using it to better understand a client’s relational patterns rather than letting it cloud the clinical picture.
Risks of unmanaged countertransference:
- Therapist avoids challenging the client on important issues
- Over-identification leads to poor boundary setting
- Therapist projects their own values or fears onto the client’s decisions
- Negative reactions cause premature termination or referral
- Client feels judged, dismissed, or misunderstood
Benefits of well-managed countertransference:
- Therapist gains real-time insight into how the client affects others in their life
- Emotional reactions serve as a diagnostic signal for underlying patterns
- Deepens the therapeutic alliance and trust
- Helps the client feel genuinely understood rather than processed
| Factor | Risk | Benefit |
|---|---|---|
| Therapist awareness | Low awareness = blind spots | High awareness = richer insight |
| Emotional reaction | Unchecked = distorted judgment | Examined = clinical data |
| Client relationship | Ignored = rupture | Addressed = stronger alliance |
For clients who want to track your mental health progress, understanding that your therapist’s self-monitoring is part of what keeps your therapy on track is genuinely useful context.
Managing countertransference: Best practices for clients and professionals
Recognizing countertransference is only half the work. The other half is doing something constructive with it. Fortunately, the field has developed solid, evidence-based approaches that work for both therapists and clients.
Management strategies include self-awareness, supervision, personal therapy, mindfulness, bracketing emotions, conceptualizing the client’s patterns, and setting clear boundaries. The guiding principle is to approach countertransference with curiosity rather than avoidance.
For mental health professionals, best practices include:
- Reflective journaling: Writing about emotional reactions after sessions helps identify patterns over time
- Clinical supervision: Regular consultation with a supervisor creates a structured space to examine countertransference without judgment
- Personal therapy: Many effective therapists remain in their own therapy to process ongoing reactions
- Mindfulness practice: Pausing before responding in session allows space to notice what is being felt and why
- Bracketing: Temporarily setting aside personal reactions to stay present with the client’s experience
For clients, knowing what to expect from a skilled therapist is empowering. You should feel that your therapist is present, curious, and not reactive. If something feels off, you have every right to bring it up.
“The goal is not to eliminate emotional reactions but to understand them well enough that they inform rather than distort the work.”
Pro Tip: If you are working through something particularly intense, understanding the basics of managing therapy-related anxiety can help you stay engaged even when sessions feel emotionally demanding.
Special challenges: Countertransference in trauma and complex cases
Even the most self-aware therapist will find that certain cases push countertransference to its limits. Trauma therapy is the clearest example. When a client shares experiences of abuse, violence, or severe loss, the therapist’s nervous system responds, often in ways that are physical, not just emotional.
Countertransference is heightened in trauma and CPTSD therapy, narcissism presentations, value conflicts, situations involving similar lived experiences, and cases involving erotic attraction. These reactions can manifest somatically, as physical tension, fatigue, or even dread before a session begins.
Common high-intensity countertransference triggers include:
- Shared trauma history: A therapist who has experienced similar trauma may over-identify with the client or avoid painful material
- Value conflicts: Clients whose choices conflict with the therapist’s core beliefs can trigger subtle judgment or withdrawal
- Narcissistic presentations: Grandiose clients may evoke contempt; vulnerable clients may evoke excessive pity
- Erotic attraction: One of the most ethically complex forms, requiring immediate supervision and clear boundary reinforcement
- Vicarious traumatization: Repeated exposure to trauma narratives can accumulate into the therapist’s own stress response
For clients navigating trauma, understanding that your therapist is actively managing their own responses is part of what makes trauma therapy safe and effective. The therapist’s role in trauma recovery includes not just technique but also ongoing emotional regulation and self-monitoring.
In these complex cases, supervision is not optional. It is essential. Peer consultation, structured debriefing, and sometimes the therapist’s own personal therapy form a protective framework that keeps the client’s care at the center.
A fresh look: Why embracing countertransference leads to better therapy
Conventional advice in clinical training often urges therapists to minimize countertransference, to stay neutral, to keep themselves out of it. We think this framing misses something important. Trying to suppress countertransference does not make it disappear. It just drives it underground, where it operates without oversight.
The therapists we have seen do the most meaningful work are not the ones with the fewest reactions. They are the ones who have learned to read their reactions like a map. When a therapist notices a flash of irritation or an unexpected wave of sadness, that signal often points directly to something significant in the client’s relational world.
Clients sometimes worry that a therapist’s emotional response means something has gone wrong. We would flip that assumption. A therapist who feels nothing is either not fully present or not being honest. Authentic engagement means reactions will happen. The question is whether they are being examined and used well.
This is why we believe the benefits of seeking counseling go beyond technique or diagnosis. The quality of the relational space, shaped in part by how a therapist handles their own inner life, is often what makes the real difference.
Find supportive therapy that values insight and self-awareness
Now that you have a clearer picture of countertransference, you might be thinking about what this means for your own therapy experience. Finding a therapist who is not just skilled in technique but also deeply self-aware makes a real difference in the quality of care you receive.
At Bergen County Therapist, Dr. Stephen Oreski and our team prioritize relational insight and professional self-reflection as core parts of effective care. Whether you are looking to explore psychotherapy options or are ready to start therapy with guidance, we offer free consultations to help you find the right fit. Both in-person and online therapy options are available, so support is accessible wherever you are in your journey.
Frequently asked questions
Can countertransference be avoided completely in therapy?
No, countertransference cannot be eliminated, but effective therapists recognize and manage it to improve outcomes. In non-psychoanalytic approaches, it is often understood simply as ordinary emotional reactions that require awareness.
How can I tell if my therapist is managing countertransference well?
If your therapist remains objective, open, and responsive rather than distracted or overly emotional, they are likely managing it skillfully. Effective therapists monitor their own reactions to stay present and use them to better understand your relational patterns.
Why is countertransference more intense in trauma therapy?
Trauma cases often stir up powerful emotions and past experiences in therapists, making countertransference more likely and noticeable. Heightened reactions in trauma therapy can even manifest physically, as tension, fatigue, or emotional dread before sessions.
What should I do if I notice a strong emotional reaction from my therapist?
It is appropriate to voice your observation in session. A skilled therapist will welcome the discussion and use it constructively rather than becoming defensive or dismissive.
Recommended
- Individual Therapy: Transforming Personal Challenges
- Role of Therapist in Trauma Recovery: Keys to Healing
- Why Seek Therapy After Narcissist – Reclaim Your Self
- CBT for Trauma: How It Transforms Healing
- Why Naming Your Feelings Helps — The Caia Journal