You don’t have to experience trauma firsthand to carry its weight. Therapists, caregivers, nurses, and first responders absorb the pain of the people they help, and over time, that exposure can fundamentally change how they see the world. This is vicarious trauma (VT), and it’s far more common than most helping professionals realize. According to researchers, vicarious trauma is a profound shift in worldview, identity, and sense of safety caused by empathic engagement with traumatized clients. This guide explains what VT is, how it differs from related conditions, and what you can do about it.
Vicarious Trauma Guide: Key Topics and Coping Strategies
- What is vicarious trauma?
- Vicarious trauma versus secondary trauma, compassion fatigue, and burnout
- How vicarious trauma develops: Mechanisms and risk factors
- Real-world impact: Prevalence and symptoms of vicarious trauma
- Vicarious trauma is not always negative: Growth and resilience
- Strategies for coping and prevention
- Find support and tools for managing vicarious trauma
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| VT alters worldview | Vicarious trauma changes your core beliefs and sense of safety from exposure to others’ trauma. |
| Distinct from burnout | VT is unique, affecting identity and schema, unlike burnout or compassion fatigue. |
| Prevention is possible | Careful self-care, supervision, and manageable workloads can reduce VT risk. |
| Growth possible | VT can foster resilience and compassion when supported by positive coping strategies. |
| Professional support helps | Professional therapy and peer support enable health professionals and caregivers to manage VT effectively. |
What is vicarious trauma?
Vicarious trauma is not just feeling sad after a hard session or a difficult shift. It’s a deeper, more lasting change in how you think, feel, and make sense of the world. VT is a profound shift in worldview caused by repeated exposure to others’ trauma, and it can affect anyone in a helping role.
The impact of vicarious trauma reaches across professions. Therapists, social workers, emergency medical technicians, nurses, and even journalists covering traumatic events are all vulnerable. What makes VT unique is that it doesn’t require a single dramatic event. It builds gradually through empathy and repeated contact with trauma narratives.
Common ways VT shows up include:
- A growing sense that the world is unsafe or unpredictable
- Difficulty trusting others, even outside of work
- Feeling emotionally detached or numb
- Questioning your sense of purpose or identity
- Intrusive thoughts or images from clients’ stories
“Vicarious trauma represents a transformation in the helper’s inner world, not just a temporary emotional reaction.”
Recognizing these signs early is the first step toward protecting your mental health and continuing to do meaningful work.
Vicarious trauma versus secondary trauma, compassion fatigue, and burnout
These four terms often get used interchangeably, but they describe different experiences. Understanding the distinctions helps you identify what you’re actually dealing with, which matters for choosing the right response.
VT is distinct from secondary traumatic stress (STS), compassion fatigue (CF), and burnout, even though they can overlap. Here’s how they compare:
| Condition | Core feature | Onset | Reversibility |
|---|---|---|---|
| Vicarious trauma | Shift in core beliefs and worldview | Gradual | Slow, requires deep work |
| Secondary traumatic stress | PTSD-like symptoms (intrusion, avoidance) | Can be sudden | Moderate with treatment |
| Compassion fatigue | Emotional exhaustion from caring | Gradual | Faster with rest and support |
| Burnout | Chronic workplace stress and disengagement | Gradual | Moderate with systemic change |
Key differences to keep in mind:
- STS involves intrusive thoughts, nightmares, and hyperarousal, much like PTSD
- CF is primarily about emotional depletion from giving too much care
- Burnout stems from organizational and workload pressures, not necessarily trauma content
- VT goes deeper, reshaping your fundamental assumptions about safety, trust, and meaning
Pro Tip: If you’re unsure which condition applies to you, consider whether your core beliefs about the world have changed. If you now see the world as fundamentally dangerous or people as untrustworthy, VT may be the more accurate label. Reviewing trauma therapy definitions can also help clarify your experience.
Personal trauma history is a strong predictor of both VT and STS. If you’ve experienced trauma yourself, your nervous system may be more reactive to the trauma content you encounter at work.
How vicarious trauma develops: Mechanisms and risk factors
VT doesn’t happen overnight. It builds through a specific psychological process. VT arises through empathy and the constructivist interaction between your personal history, coping strategies, and repeated exposure to clients’ trauma narratives. In other words, your own life experiences shape how deeply trauma content affects you.
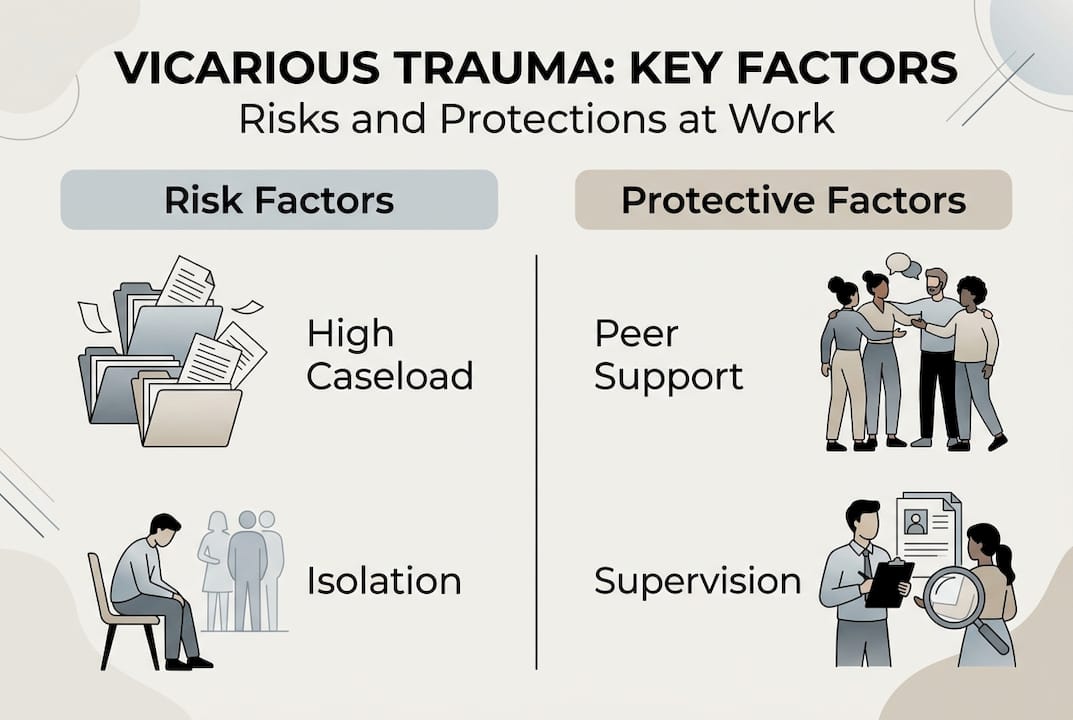
Here are the main risk factors that increase vulnerability to VT:
- High caseloads with limited time for recovery between sessions
- Lack of clinical supervision or peer support
- Personal history of unresolved trauma
- Low self-compassion and harsh self-criticism
- Work overload with little control over schedule or boundaries
Risk factors include high caseloads, lack of supervision, personal trauma history, and low self-compassion, while protective factors include supervision, experience, self-compassion, and regular exercise.
| Factor type | Examples |
|---|---|
| Risk factors | High caseload, no supervision, trauma history, isolation |
| Protective factors | Regular supervision, peer support, self-compassion, and exercise |
If you’re wondering whether your current work environment is putting you at risk, choosing a trauma therapist who understands occupational trauma can be a valuable step. Understanding the therapist’s role in recovery also helps clarify what kind of support is most effective. For those working with younger populations, child trauma therapy carries its own unique emotional demands.
Statistic to know: Prevalence rates of VT symptoms vary widely by profession and region, which means your risk level is not fixed. It depends heavily on your work context and the support systems around you.
Real-world impact: Prevalence and symptoms of vicarious trauma
VT is not rare. It’s a widespread occupational hazard in helping professions, and the numbers reflect that reality. Prevalence of VT symptoms among mental health professionals ranges from 21% to 74%, with rates even higher in developing countries. Among trauma nurses specifically, 35.9% report burnout, 27.3% report compassion fatigue, and 7% report secondary traumatic stress.
Symptoms of VT can be subtle at first, then intensify over time:
- Emotional numbness: Feeling disconnected from clients, loved ones, or your own emotions
- Irritability: Shorter fuse, less patience, more reactive in personal relationships
- Worldview shifts: Growing cynicism, loss of faith in people or systems
- Loss of safety: Feeling that danger is everywhere, even in ordinary situations
- Identity disruption: Questioning your purpose, values, or sense of self
“When the stories you carry start to feel like your own, that’s when VT has taken hold.”
If several of these symptoms feel familiar, you’re not alone, and you’re not weak. VT is a predictable response to sustained empathic exposure. Exploring a trauma healing guide can help you understand what recovery actually looks like.
Vicarious trauma is not always negative: Growth and resilience
Here’s something that surprises many people: VT doesn’t have to end in damage. VT can lead to vicarious post-traumatic growth through reflection on clients’ resilience, and this growth is real and measurable.
Vicarious post-traumatic growth (VPTG) refers to positive psychological changes that emerge from the struggle with highly challenging circumstances. Helpers who process their experiences thoughtfully often report:
- Deeper empathy and compassion for others
- A stronger sense of personal meaning in their work
- Greater appreciation for their own relationships and life
- Increased professional skill and emotional intelligence
- A more nuanced, realistic view of human strength
Pro Tip: Growth doesn’t happen automatically. It requires intentional reflection, often with a supervisor or therapist. Simply enduring exposure without processing it leads to damage, not growth. If you’re ready to explore this path, learning about starting trauma therapy can help you take that first step.
Peer support groups, reflective journaling, and structured supervision are all evidence-backed ways to turn difficult exposure into professional and personal development.
Strategies for coping and prevention
You can take concrete steps to protect yourself from VT and build resilience over time. Caregivers and therapists should prioritize supervision, self-compassion training, manageable caseloads, and monitoring early warning signs.
Here’s a practical framework to get started:
- Seek regular supervision. Clinical supervision is not a luxury. It’s a professional necessity that reduces VT risk significantly.
- Practice self-compassion. Treat yourself with the same care you extend to clients. Self-criticism accelerates burnout and VT.
- Manage your caseload. Set realistic limits on the number of high-trauma clients you see per week.
- Build a peer support network. Talking with colleagues who understand your work reduces isolation and normalizes your experience.
- Exercise regularly. Physical activity is one of the most consistently supported protective factors in the research.
- Recognize early warning signs. Catch VT before it becomes entrenched by checking in with yourself weekly.
Additional self-care practices that help:
- Maintain clear boundaries between work and personal life
- Engage in activities that restore your sense of joy and safety
- Limit after-hours contact with clients when possible
- Use grounding techniques after difficult sessions
Understanding the role of trauma therapy in your own life, not just your clients’ lives, is a powerful reframe. Helpers need help too, and seeking it is a sign of professional maturity, not weakness.
Find support and tools for managing vicarious trauma
Knowing the strategies is one thing. Having the right support to actually use them is another.
At Bergen County Therapist, Dr. Stephen Oreski and his team work with caregivers, therapists, and first responders who are navigating the psychological toll of their work. Whether you’re dealing with emotional exhaustion, worldview shifts, or something harder to name, there are real options available. You can track your mental health over time to spot patterns early, explore psychotherapy options tailored to trauma-related distress, or find targeted support through depression therapy if VT has shifted into something deeper.
A free consultation is available to help you find the right fit.
Frequently asked questions
How is vicarious trauma different from burnout?
Vicarious trauma changes core beliefs and worldview, while burnout is primarily emotional and physical exhaustion driven by chronic workplace stress, not trauma content specifically.
Who is most at risk of vicarious trauma?
People with high caseloads, limited supervision, a personal trauma history, and low self-compassion face the greatest risk, including therapists, nurses, social workers, and first responders.
Can vicarious trauma be prevented?
Yes. Supervision, self-compassion, and manageable caseloads are among the most effective protective factors, especially when combined with peer support and regular self-monitoring.
What symptoms indicate vicarious trauma?
Emotional numbness, irritability, worldview shifts, and a persistent loss of sense of safety are the most common indicators that VT may be present.
Is vicarious trauma always negative?
No. When processed intentionally, VT can lead to growth in empathy, professional skill, and personal meaning, a phenomenon researchers call vicarious post-traumatic growth.
Recommended
- How trauma affects relationships: 70% face challenges
- Vicarious Trauma and Its Impact on Caregivers – Dr. Stephen Oreski & Associates
- Child Trauma Therapy: Definition, Types, and Impact
- Trauma Therapy: Healing with Dr Stephen Oreski & Associates.
- Featured Mindfulness Course | Mindful Self Compassion in Support of Psychedelic-Assisted Therapy